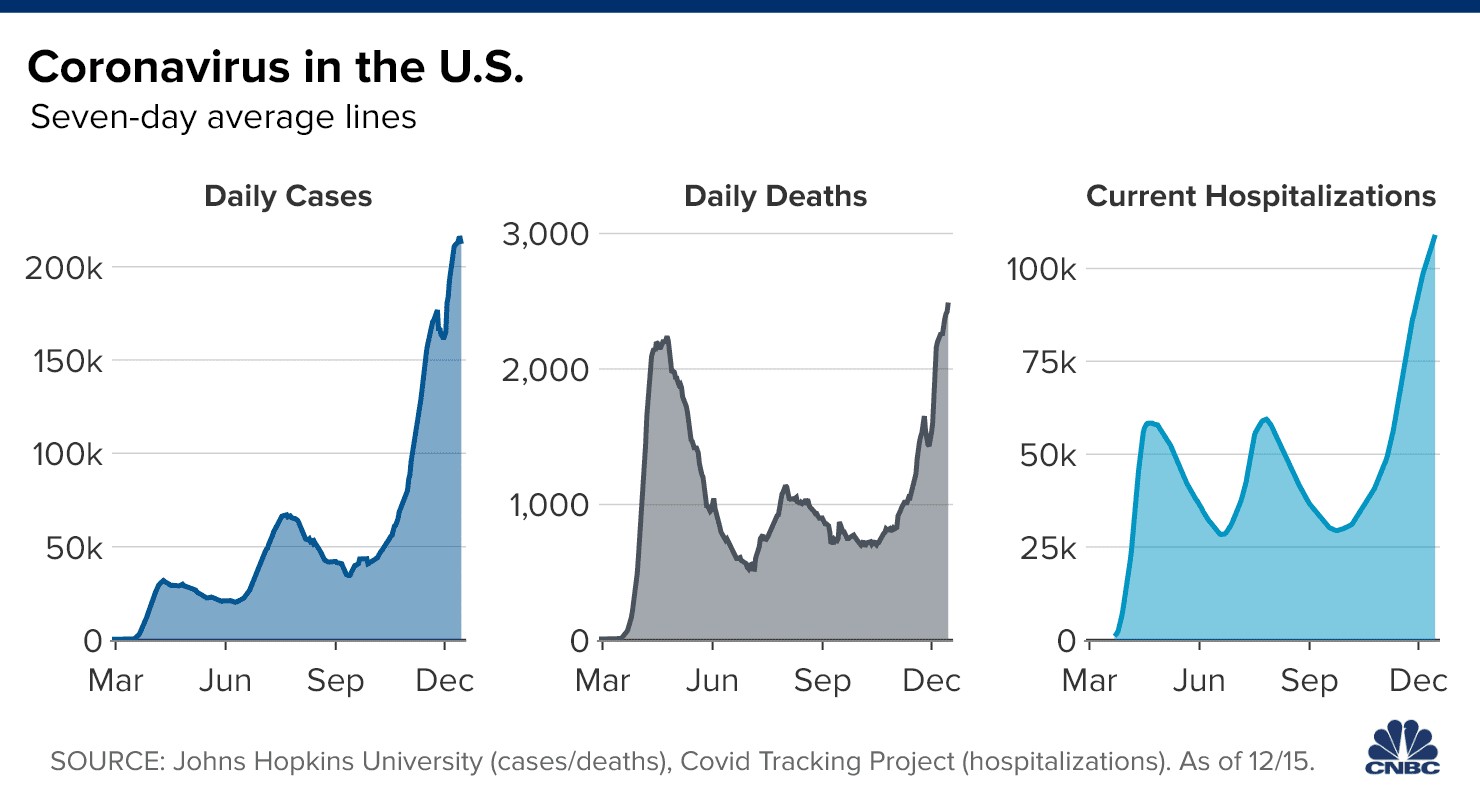
 Many hospitals and ICUs across the U.S. are at or near their highest capacity levels since the start of the pandemic. On Tuesday, 112,816 people were hospitalized with Covid-19
Many hospitals and ICUs across the U.S. are at or near their highest capacity levels since the start of the pandemic. On Tuesday, 112,816 people were hospitalized with Covid-19, according to the Covid Tracking Project, setting another record for that metric. Hospitalizations were up 7.9% over the past week and have increased nearly 61% over the past month.
https://carlsonschool.umn.edu/mili-misrc-covid19-tracking-projectA model from the University of Washington's Institute for Health Metrics and Evaluation forecasted the need for 154,835 hospital beds by Jan. 27, its predicted peak of the recent surge, and 38,004 ICU beds on Jan. 26. Hospitalizations tend to lag new Covid-19 infections by at least several weeks.
Last week, New Mexico issued two new public-health emergency orders suspending nonessential surgeries and activating “crisis care” standards.
... Russell Judd, chief executive of Kern Medical in Bakersfield, Calif., said Tuesday that
his trauma center had two empty beds in the ICU, not because there was no demand for them but because he didn’t have enough nurses to staff them. ... What’s unprecedented is that we're offering $175 an hour, and can't find a nurse that can come work for us.”----------------------------------------
California Opens COVID-19 Field Hospitals Across the Statehttps://www.latimes.com/california/story/2020-12-16/facing-a-a-grim-set-of-weeks-california-opens-covid-field-hospitals-across-the-state?_amp=trueCalifornia is opening temporary field hospitals to help with overflow patients as COVID-19 surges fill intensive care units across the state.The field hospitals will care for non-ICU patients in places such as Costa Mesa, Porterville, Sacramento and Imperial; other facilities are on standby status in Riverside, Richmond, Fresno, San Diego and San Francisco.
On Tuesday, the California Department of Public Health said available ICU capacity in Southern California was just 1.7%, down from 2.7% a day earlier. The situation was particularly grim in Riverside County, which was at zero available ICU capacity as of Tuesday. Available ICU capacity in the San Joaquin Valley was also effectively maxed out and has been fluctuating between zero and 1.6% since Saturday.
Fresno County has nearly 1 million people, but there were only 16 available ICU beds Monday. A couple of that region’s larger hospitals have zero available ICU beds, and one has been forced to keep five ICU patients in the emergency department.
Besides an alternative care site in Porterville that opened Monday, another staffed 50-bed care site is being opened this week next to Community Regional Medical Center in Fresno. That site can take patients from in-patient wards, freeing up space in the step-down units where critically ill patients recover, which in turn frees up space in the ICU.
Last week, a site was opened at Sleep Train Arena, the former home of the NBA’s Sacramento Kings. That care site, which has 20 beds available and a capacity of up to 244 beds, is currently treating seven patients. An additional 23 patients have filled available beds at Imperial Valley College, which has space for an additional 100 beds. The state also has a site for patients from the California Department of State Hospitals, which has 43 of 46 available beds filled to treat patients.
Dr. Rais Vohra, Fresno County’s interim public health officer, said Tuesday that he expected “a grim set of weeks before and after the new year, just given the trends that we’re seeing…. Unfortunately, we’ve just got a lot of infections and a lot of ongoing transmissions [and] we’re still very, very hard pressed to try to meet that challenge.”
Dr. Mark Ghaly, the California health and human services secretary, said two weeks ago that California was averaging around 15,000 cases a day, a number that has since more than doubled.
“That should tell you that in the next couple of weeks what our hospitals will be facing, the amount of people knocking on the front door with COVID to the emergency room departments that need an in-patient hospital bed, that might need that ICU bed, are going to increase,” Ghaly said.
----------------------------------------

-----------------------------------------
Health Care Worker In Alaska Has Severe Allergic Reaction to Coronavirus Vaccinehttps://www.washingtonpost.com/health/allergic-reaction-covid-vaccine-alaska/2020/12/16/cf8f5c56-3fcb-11eb-8db8-395dedaaa036_story.html?outputType=ampA health care worker in Alaska had a serious allergic reaction after getting the new coronavirus vaccine developed by Pfizer and BioNTech — the first such case reported in the United States since shots began going into arms earlier this week, state officials revealed Wednesday.
The Alaska case echoes two similar cases in the United Kingdom in which health care workers had serious but nonfatal allergic reactions to the vaccine. But the UK workers had histories of severe allergic reactions, whereas the Alaska woman had none, state health officials said. She is now stable and was discharged from a hospital where she was kept overnight.
In randomized trials, Pfizer reported no such allergic responses, known as anaphylaxis, but people with a history of such severe reactions were excluded from participating.The Alaska health care worker, described as middle-aged but otherwise not identified, began flushing and experiencing other signs of an allergic response about 10 minutes after she received the shot Tuesday afternoon at Bartlett Regional Hospital in Juneau.
---------------------------------------
elsewhere ...Kansas Mayor Resigns Over Mask Mandate Threatshttps://www.sfgate.com/business/article/The-Latest-Germany-pushes-for-quick-EU-vaccine-15802168.phpKANSAS — A western Kansas mayor announced Tuesday that she is resigning, effective immediately, because of threats she has received after she publicly supported a mask mandate.
Dodge City Mayor Joyce Warshaw said she was concerned about her safety after being met with aggression, including threats via phone and email, after she was quoted on a
USA Today article on Friday supporting the mandate, ]I]The Dodge City Globe[/I] reported.
“I understand people are under a lot of pressure from various things that are happening around society like the pandemic, the politics, the economy, so on and so forth, but I also believe that during these times people are acting not as they normally would,” Warshaw said.
Ford County, where Dodge City is located, has recorded 4,914 cases of COVID-19 since the pandemic began, according to the state health department. The county has about 33,600 residents
--------------------------------------
Pfizer Vaccine Shipments in California, Alabama Got Too Cold, Vials Had to be Quarantined and Replacedhttps://www.cnbc.com/2020/12/16/covid-vaccine-us-quarantines-pfizer-shipments-in-california-alabama-after-transit-anomaly.htmlU.S. officials quarantined Pfizer coronavirus vaccine shipments in California and Alabama after they said a transit issue left the vials too cold.
Pfizer’s vaccine requires a storage temperature of around minus 70 degrees Celsius. Vials of the vaccine are stored in trays, which carry a minimum of 975 doses each, according to the CDC.
Gen. Gustave Perna, who oversees logistics for Operation Warp Speed, told reporters that two trays of vaccine that arrived in California had to be returned to Pfizer after the temperature somehow fell to minus 92 degrees Celsius. He said the “anomaly” happened again in Alabama.
“All the way on the other side of the country in Alabama, two trays were received at one location. Same anomaly, went to minus 92. We were able to stop and quarantine the vaccine, stop and get a replacement shipment to Alabama,” he said.
------------------------------------------
Health Experts Are Concerned Prisoners Have Been Excluded From Vaccine Planshttps://www.cnbc.com/2020/12/16/coronavirus-prisoners-have-been-excluded-from-covid-vaccine-plans.htmlHealth experts and criminal justice advocates have expressed deep concern over the notable absence of prison populations among coronavirus inoculation plans.
“If the biggest hotspots for Covid are prisons, doesn’t it make sense to inoculate everyone from the guards to the prisoners?” said Ashish Prashar, a justice reform advocate and senior director of global communications at Publicis.
Health officials have been warning about the dangers of epidemics for those incarcerated for years, citing an inability for people to maintain safe physical distancing in correctional facilities because of their confinement in small shared spaces.
